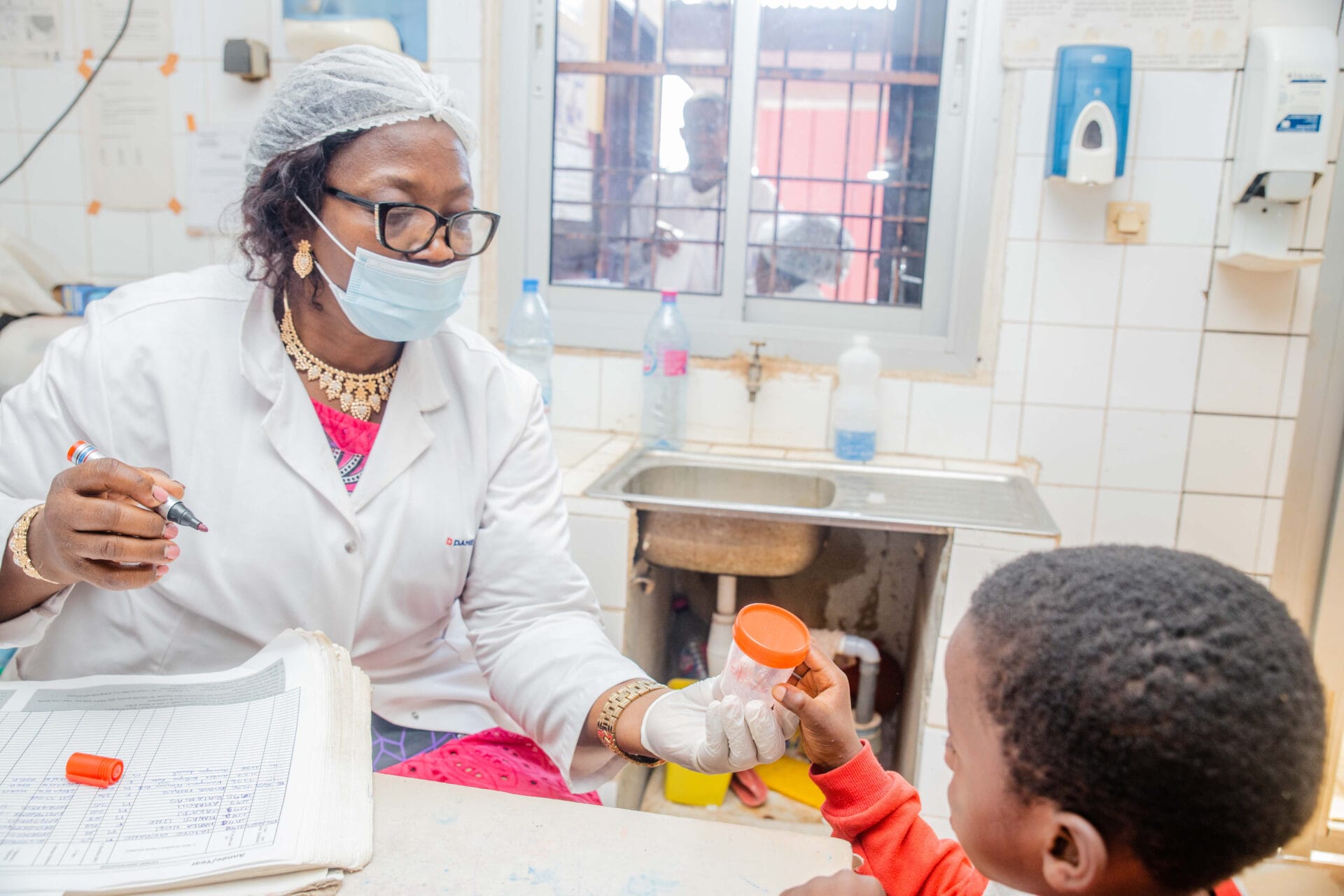
Giving community health workers a greater role in the Greater Mekong subregion
Between 2012 and 2015, the incidence of malaria in the Greater Mekong subregion fell by 54% to less than 300,000 annual cases, while deaths fell by 84%. Nevertheless, in parts of the Greater Mekong subregion, Plasmodium falciparum, the deadliest species of malaria parasite, has developed resistance to several artemisinin-based combination therapies, which is currently the most effective treatment available.
A global approach to a regional threat
This drug resistance was first observed in Cambodia and Thailand, and later in Burma, Laos, and Vietnam. These five countries, which face similar challenges—migration and population mobility, ethnic minorities, hard-to-reach areas—therefore joined the Regional Artemisinin-Resistance Initiative (RAI) in 2014, of which L’Initiative is also a partner. Financed by a Global Fund grant, the RAI closely monitors malaria cases. It is supported by a civil society organization coordination platform, a network of around 40,000 community health workers, many of whom are volunteers, who work in the villages and the region’s rural and forested areas.
Rolling out community services
These workers report detected cases using a smartphone application that updates the national database in real-time, facilitating a rapid response in the event of a localized epidemic. As a key link between the most vulnerable population groups and healthcare systems, community health workers are central to the regional monitoring system. Their role is crucial since early diagnosis and treatment are essential to eliminating malaria. Training them is, therefore, a priority for the RAI.
In countries with a severe shortage of health professionals, they bridge the gap and improve prevention, access to screening, and the quality of care, particularly in places that are hard to reach or far from health centers. Communities also trust community workers. They play an important role in promoting health and in preventing infectious diseases, which are viewed in different ways depending on the communities’ cultural contexts.
Aligning the regional community response
The number of volunteers, their services, the financial incentives they receive, and their status within healthcare systems vary greatly between countries. While in Cambodia, Laos, and Burma, they are the backbone of malaria diagnosis and treatment, more stringent national regulations in Thailand and Vietnam prevent many community health workers from providing such diagnosis and care. This results in unequal treatment and access to health equipment and materials, hampering regional-level volunteer network coordination and management. This also affects the development of a sustainable regional community strategy.
A recent report on the role of community health workers in the RAI region therefore recommends better integrating such workers into the five countries’ healthcare systems to improve their working conditions, provide them with a decent salary, and give them better training. The report suggests community health workers should also treat other health concerns affecting communities, such as diarrhea, malnutrition, and respiratory infections. This would step up their prevention and awareness-raising role and would involve them in patient referral to primary care facilities. Lastly, the report proposes developing national roadmaps to strengthen the regional coordination of community health worker networks so as to harmonize their functions and deployment in the various countries.